While less common than other symptoms, yes, uterine fibroids can cause blood in the urine (hematuria). This usually happens when larger fibroids press directly on your bladder or nearby urinary structures, triggering irritation or blockage. If you notice blood, always see your doctor for a clear diagnosis.
Seeing blood in your urine can be startling, and it’s totally normal to feel worried. You might be wondering if something serious is going on, especially if you already know you have uterine fibroids. Think of this as a simple guide to help you understand the connection—or lack thereof—between these two things. We are going to break down exactly why this might happen in plain, easy-to-understand language.
You don’t need fancy medical knowledge to grasp this! We’ll explain the plumbing, look at the signs, and guide you on what steps feel right and supportive for your health. By the end of this read, you will feel much more confident about what might be causing this symptom and what to discuss with your healthcare provider.
Decoding the Connection: Do Fibroids Cause Blood In Urine?
This is the million-dollar question! The simple answer is: sometimes, yes, but usually indirectly. Uterine fibroids are non-cancerous growths in or on the muscles of the uterus. They often cause heavy periods or pelvic pressure, but their effect on your urinary tract isn’t always immediate.
To understand the link, we must first understand where everything sits in your body. Your uterus, bladder, and ureters (the tubes draining urine from the kidneys) are all located very close together in the pelvis. When a fibroid grows quite large, or if it grows in a specific location, it can start bumping into or pushing on these delicate urinary parts.
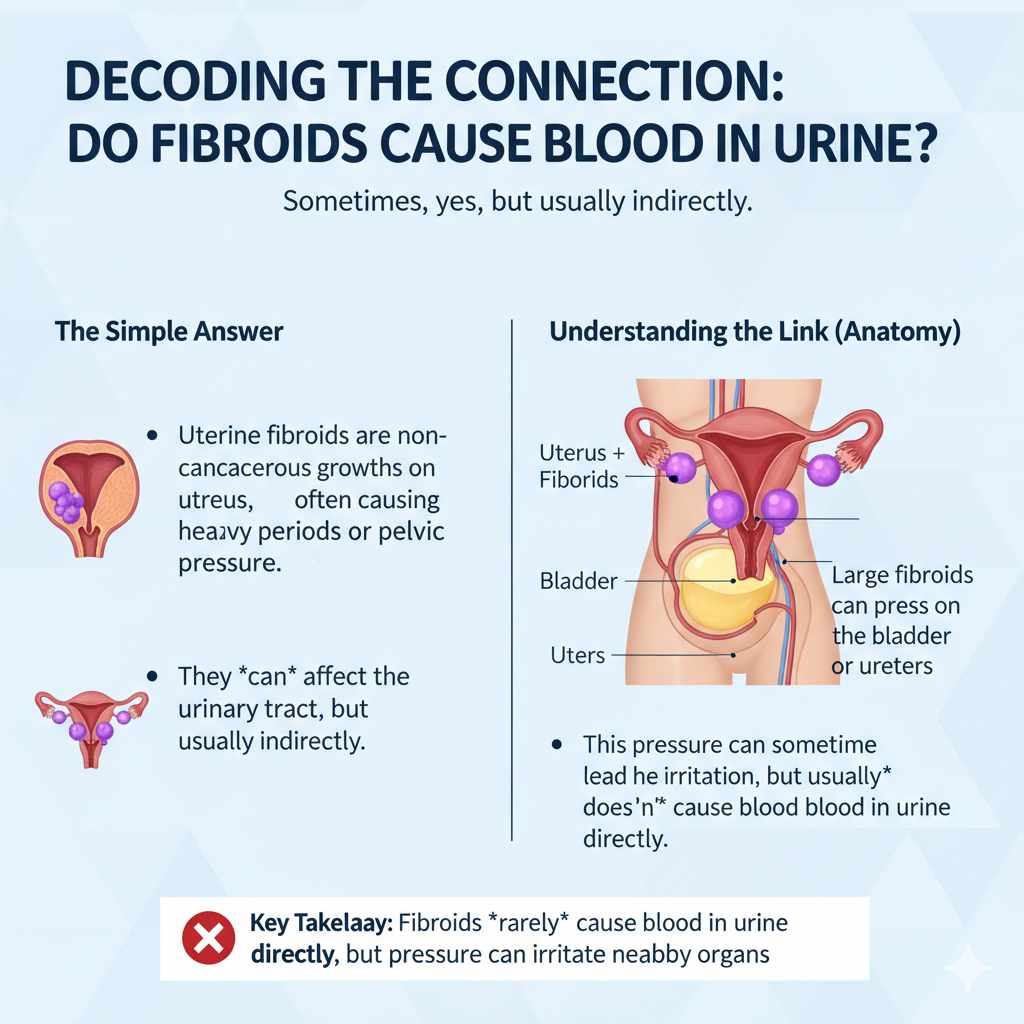
How Fibroids Interact with the Urinary Tract
Fibroids primarily affect menstruation. However, proximity leads to problems. When a fibroid presses on an established structure, that structure can become irritated, inflamed, or partially blocked. This irritation is often the gateway for blood to appear where it shouldn’t.
Here are the primary ways fibroids impact the urinary system:
- Direct Bladder Pressure: Large, anterior (front-facing) fibroids can press squarely against the bladder wall. This constant pressure can cause microscopic tears or inflammation, leading to blood in the urine.
- Ureteral Obstruction: If a fibroid grows outside the uterus and presses on a ureter, it can block the flow of urine from the kidney down to the bladder. This backup causes pressure in the kidney, which can sometimes result in visible blood (hematuria).
- Structural Change: Very large fibroids can actually distort the entire shape of the pelvic cavity, putting stress on the surrounding plumbing systems, even without direct contact.
Understanding Hematuria: Blood in Your Urine
The medical term for seeing blood in your urine is hematuria. Don’t panic if you see a pink, red, or cola-colored tinge in the toilet bowl. It’s a symptom that needs investigation, not a diagnosis in itself. It simply tells us something is irritated or damaged somewhere along the urinary path.
What Does Hematuria Look Like?
Hematuria can show up in different ways. Knowing the difference can help you describe the symptom clearly to your doctor. Imagine it like paint splatters—sometimes just a drop, sometimes a flood!
| Type of Hematuria | Appearance | What It Means (Generally) |
|---|---|---|
| Gross Hematuria | Urine appears distinctly pink, red, or brown (like tea or cola). You can see it without a microscope. | Indicates a significant amount of bleeding occurring in the urinary tract. |
| Microscopic Hematuria | Urine looks normal, but blood cells are found during a urine test (urinalysis). | May indicate very mild irritation or an early issue. |
If you have fibroids, you are already dealing with pelvic changes. It is crucial to remember that while fibroids might be the culprit, other things can cause blood in the urine, too! Think of it like a guest list—fibroids are invited, but so are infections and other conditions.
Other Common Causes of Blood in Urine
When you visit your healthcare provider, they will run tests to rule out these other common issues, which often present similarly to fibroid-related urinary bleeding:
- Urinary Tract Infections (UTIs): These are very common and cause bladder inflammation, often leading to pink or bloody urine alongside burning or urgent need to go.
- Kidney Stones or Bladder Stones: As stones move, they scrape the delicate lining, causing bright red blood.
- Kidney Disease: Certain kidney issues can cause leakage of red blood cells.
- Bladder or Kidney Cancer: While rare, this is why any unexplained hematuria must be checked by a professional.
- Vigorous Exercise: Intense physical activity can sometimes cause temporary, minor bleeding.
This checklist shows why professional confirmation is essential. We want to make sure we are truly tackling a fibroid issue rather than something else that needs different care.
When Do Fibroids Start Causing Urinary Symptoms?
The size and location of the fibroid are the biggest determining factors. A small fibroid tucked against the back wall of the uterus might never bother your bladder. But a medium-sized one growing toward the front can cause trouble even if it’s not giant.
Key Factors Influencing Symptom Onset
- Size Threshold: Fibroids usually need to reach a certain size—often several centimeters in diameter—before they exert enough physical mass to press significantly on the bladder.
- Location, Location, Location: A submucosal fibroid (growing just under the lining) is unlikely to affect urine flow unless it’s massive. A pedunculated fibroid (hanging on a stalk) near the bladder might cause intermittent irritation if it swings or shifts.
- Uterine Changes: As the uterus grows larger due to multiple fibroids, the overall pressure in the pelvis increases, making the bladder more vulnerable to irritation.
For many women, the major urinary symptom associated with fibroids isn’t blood, but rather frequency (feeling like you have to pee constantly) or urgency. Blood in the urine suggests a more direct irritation or damage point has been reached.
Your Action Plan: What to Do If You See Blood in Your Urine
Seeing blood is your body sending a clear signal. As a homeowner, when you see a worrying stain, you don’t ignore it; you call in the experts for a proper inspection. This is the same approach for your health!
Step 1: Stay Calm and Note the Details
Before you call the doctor, take a moment to gather helpful information. This helps speed up the diagnostic process.
- Color Check: Is it pink, bright red, or dark brown/cola colored?
- Timing: Did it happen just once, or is it happening every time you urinate?
- Accompanying Symptoms: Are you also experiencing pain, fever, painful urination (dysuria), or heavy menstrual bleeding?
- Medication Review: Are you taking any new medications? (Though rare, some common drugs like the laxative Senna or beetroot consumption can change urine color, mimicking blood.)
Step 2: Schedule a Prompt Appointment
Because there are many causes for hematuria, you need a professional evaluation. Call your primary care physician or gynecologist right away. If the bleeding is extremely heavy, accompanied by severe pain, or if you develop a fever, seek urgent care.
Step 3: Prepare for Diagnostic Tests
Your doctor will use simple, non-invasive tests first to pinpoint the source of the bleeding. This is much like checking the foundation before redecorating!
Common tests include:
- Urinalysis: A simple dipstick test of your urine to confirm the presence of red blood cells and check for signs of infection (bacteria or white blood cells).
- Urine Culture: If infection is suspected, this test identifies the specific bacteria present.
- Imaging Scans: Since you may already know about fibroids, an ultrasound (which you might have had before) or a CT scan can specifically show the size, number, and exact location of your fibroids relative to your bladder.
Medical Management: Treating Fibroid-Related Hematuria
If the tests confirm that the fibroids pressing on your bladder are indeed the cause of the blood in your urine, the treatment path focuses on shrinking the fibroids or relieving the pressure they cause.
Non-Surgical Relief Options
If the bleeding is mild and caused by irritation, your doctor might suggest managing the symptoms first while monitoring the fibroids.
| Treatment Approach | How It Helps Urinary Symptoms | Best For |
|---|---|---|
| Hormonal Birth Control | Can reduce overall fibroid size slightly and regulate cycles, lessening pelvic bulk. | Smaller fibroids causing mild, infrequent urinary irritation. |
| GnRH Agonists (e.g., Lupron) | These temporarily shut down ovarian function, causing fibroids to shrink significantly. | Preparing for surgery or severe, short-term relief. They are usually not a long-term solution due to side effects. |
It is important to check reputable sources for the latest information on fibroid therapies. Organizations like the U.S. Office on Women’s Health offer clear, vetted data on treatment options.
When Intervention is Necessary
If the fibroids are large enough to cause persistent hematuria, significant pain, or blockages leading to kidney problems, reducing their size may become necessary. This is where more direct interventions come into play:
- Uterine Fibroid Embolization (UFE): A specialist blocks the blood supply to the fibroids, causing them to starve and shrink. This often relieves pressure on surrounding organs like the bladder.
- MRI-Guided Focused Ultrasound Surgery (MRgFUS): Sound waves are used to heat and destroy fibroid tissue without incisions.
- Myomectomy: A surgical procedure to selectively remove the fibroids while leaving the uterus intact. If the bothersome fibroid is removed, the pressure on the bladder is immediately relieved, and bleeding should resolve.
Style Your Health: Prioritizing Comfort and Communication
As someone who loves making a home beautiful and comfortable, you understand that sometimes a minor tweak fixes a major annoying issue. Treating your health situation similarly means finding the right solution to restore your comfort. A healthy body is the foundation for a beautiful, well-lived home!
Communicating Clearly with Your Healthcare Team
Think of your doctor’s visit like a design consultation. You need to clearly articulate the “problem area” so they can propose the right “fix.” Don’t downplay symptoms out of embarrassment or hope they go away.
Use these prompts as talking points:
- “I have confirmed uterine fibroids, and recently I have noticed [color/frequency] of blood when I urinate.”
- “The urinary symptom seems worse after exercising/at the end of the day/when my period starts.”
- “I want to rule out a UTI or a stone, but I am concerned the fibroid pressure is the root issue.”
Remember, your quality of life matters. Just as you wouldn’t tolerate a drafty window forever, you shouldn’t have to live with bothersome urinary symptoms if a manageable solution exists.

Frequently Asked Questions (FAQ) for Beginners
Q1: If I have heavy periods because of fibroids, does that mean I will also have blood in my urine?
A: Not necessarily. Heavy periods happen because fibroids affect the uterus’s surface area, causing more cramping and bleeding there. Blood in urine comes from pressure or irritation to the bladder or ureters, which is a separate plumbing issue.
Q2: How long after a fibroid grows will it start causing urinary symptoms?
A: There is no set timeline. It depends entirely on the fibroid’s direction of growth. A fibroid can grow large for years without affecting the bladder, or a smaller one, if perfectly positioned near the bladder neck, could cause issues quickly.
Q3: If my urine is dark brown (like coffee) instead of red, could fibroids still be the cause?
A: Dark brown or cola-colored urine usually suggests bleeding higher up in the urinary tract, often from the kidneys, or it can indicate severe bleeding that has oxidized. Since fibroids can press on the ureters leading from the kidneys, this is certainly a possibility that needs immediate medical review.
Q4: Is blood in the urine from fibroids painful?
A: Sometimes it is painless (microscopic hematuria). If the fibroid is severely obstructing a ureter, causing pressure backup in the kidney, that can result in very intense, sharp flank pain that radiates downward, along with the blood.
Q5: Can I manage fibroid-related blood in urine naturally?
A: While lifestyle changes support overall pelvic health, they generally won’t shrink a large fibroid that is physically pressing on the bladder. If the bleeding is mild irritation, stress reduction and staying hydrated help, but for confirmed pressure symptoms, medical advice on shrinking the growth is usually required.
Q6: If I get a hysterectomy to remove the uterus (and fibroids), will the blood in urine stop?
A: If the blood in urine was directly and solely caused by the fibroids pressing on the bladder, then yes, removing the source of the pressure (your uterus) should resolve the urinary symptom. However, your doctor will confirm this is the cause before surgery.
Conclusion: Moving Forward with Clarity
We’ve covered a lot of ground today, and hopefully, you feel much clearer about the sometimes confusing signals your body sends. Remember, while uterine fibroids are very common—affecting up to 80% of women by age 50—seeing blood in your urine is never normal and always warrants a check-up. It’s an important piece of data about what’s happening in your pelvic space.
If your fibroids are the culprits, dealing with fibroid-related hematuria is about finding the right treatment pathway to remove that pressure. Whether that means monitoring, medication to shrink the growths, or a targeted procedure, the goal is always the same: restoring your comfort and peace of mind. Don’t hesitate to partner with your doctor, armed with the knowledge you gained here, to design a health plan that lets you get back to enjoying the beautiful, comfortable spaces you create in your life!